Why 3D Body Maps Are Changing Dermatology Documentation
Read Time 7 mins | Aug 21, 2025 10:13:00 AM | Written by: Dr. Srdjan Prodanovich, MD, FAAD
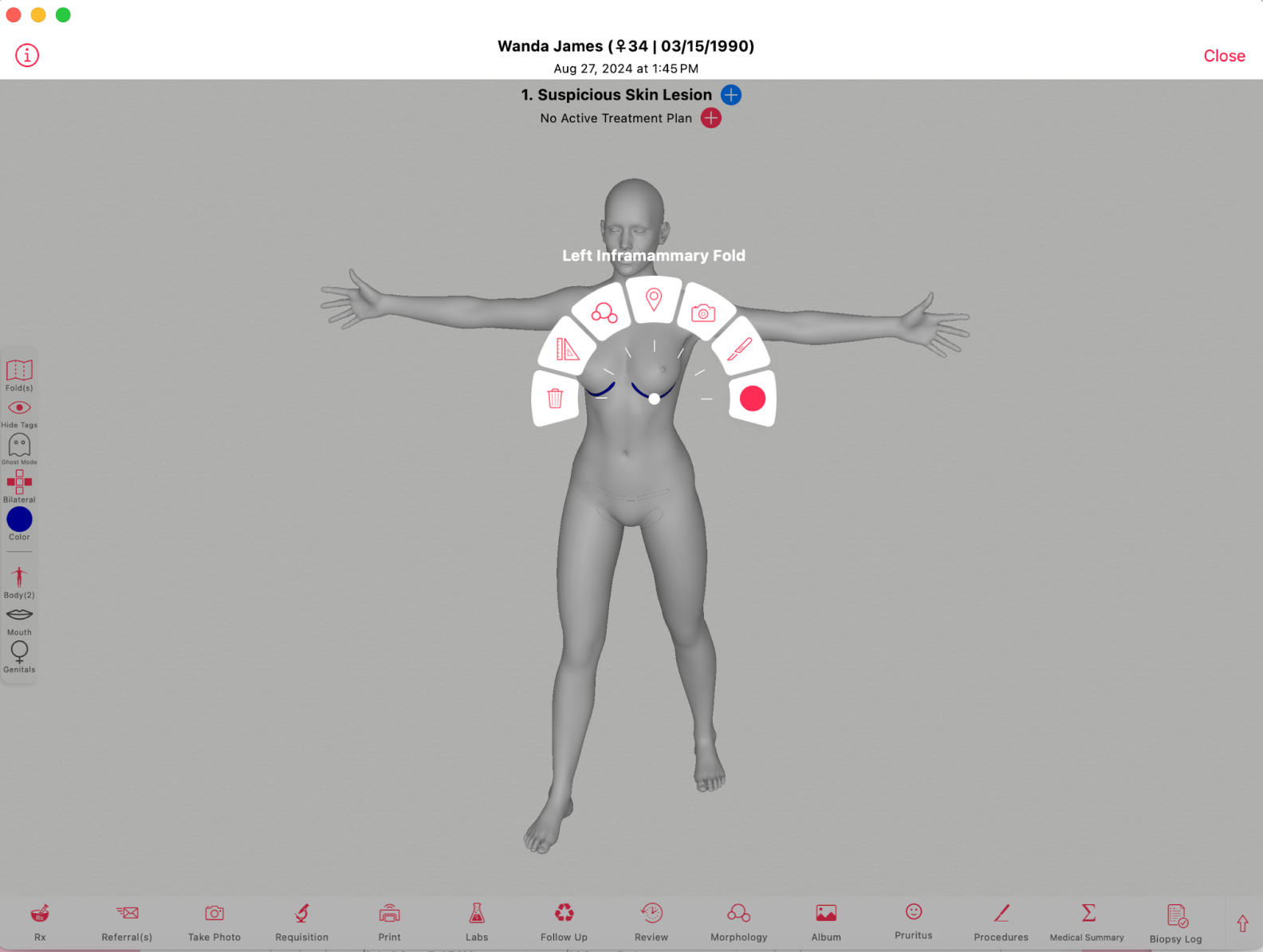
Traditional 2D body maps and narrative notes often leave dermatologists questioning whether a lesion has changed, or if it’s even the same one documented at the last visit. This uncertainty leads to unnecessary biopsies, patient anxiety, and wasted time.
3D body maps are transforming dermatology EHRs by providing precision documentation, longitudinal lesion tracking, and structured coding. For dermatologists, this means not just better care but also stronger compliance, reduced liability, and improved efficiency across the entire practice.
Table of Contents
- What Is a 3D Body Map in Dermatology EHR?
- How 3D Body Maps Improves Diagnostic Precision
- Earlier Melanoma Detection Through Longitudinal Tracking
- Reducing Unnecessary Biopsies and Patient Anxiety
- Better Communication Across Providers and Pathology
- Stronger Billing, Compliance, and Legal Protection
- How 3D Body Maps Engage Patients in Their Own Care
- FAQ
- Key Takeaways
- Conclusion
What Is a 3D Body Map in Dermatology EHR?
A 3D body map is an interactive, coded documentation tool that allows dermatologists to pinpoint lesions with exact anatomic accuracy. Instead of writing "left arm," providers can document "proximal dorsal forearm, adjacent to the olecranon," removing ambiguity and improving long-term tracking.
This precision goes far beyond what flat, 2D body maps can provide. For example, documenting a lesion behind the ear, between the fingers, or even inside the oral cavity is nearly impossible with a simple flat drawing. With 3D body maps, these hard-to-represent areas can be localized exactly where they are, eliminating ambiguity and ensuring reproducible documentation.
Case example: A patient comes in after two years with a concern about a mole behind the ear. On a 2D body map, the documentation might have been “left ear,” which could be interpreted differently by another provider. With a 3D body map, the exact location on the posterior auricular surface is clear, removing doubt and protecting against misidentification.
How 3D Body Maps Improves Diagnostic Precision
Precise localization prevents confusion about lesion identity. Dermatologists can correlate changes across visits with confidence, and documentation becomes reproducible across different clinicians.
Instead of guessing if a mole is the same as last year, providers can reference previously documented lesions and instantly see whether it has changed in size, shape, or location. This clarity is particularly critical in areas like between the fingers or inside the mouth, where even small changes are difficult to chart using a 2D body map. Charting on a 3D body map allows providers to zoom in, rotate, and document with exact precision.
Case example: A teenage patient with numerous atypical nevi is seen by different providers in a group practice. Thanks to 3D body maps, each dermatologist can see exactly which lesions were documented previously, including one tucked between the fingers, ensuring consistent monitoring across visits.
Earlier Melanoma Detection Through Longitudinal Tracking
Melanomas often appear as subtle changes over time. With a 3D body map, dermatologists can quickly spot:
- Newly developed nevi: Fresh lesions can be immediately distinguished from pre-existing ones, allowing providers to focus on what is truly new and potentially suspicious.
- Morphologic changes: Alterations in color, border irregularity, or asymmetry are flagged in context, rather than relying on imperfect memory or vague notes.
- Lesion growth that warrants biopsy: Measurable increases in size can be tracked precisely, making the decision to biopsy more evidence-based.
This longitudinal view empowers dermatologists to detect malignancies at their earliest and most treatable stages. It is especially valuable for sites that are often overlooked in flat diagrams, like behind the ear or on mucosal surfaces, where subtle but dangerous changes can otherwise go unnoticed.
Case example: A patient returns after 18 months, and the dermatologist references the previously documented photos on the 3D body map from the prior visit. A mole in the oral mucosa, documented precisely on the 3D map, now shows subtle enlargement. Because the change is clearly demonstrated, the provider biopsies it and catches melanoma at an early, curable stage.
Reducing Unnecessary Biopsies and Patient Anxiety
Without clear lesion history, biopsies are often performed “just to be safe.” 3D mapping reduces this uncertainty, meaning fewer:
- Unnecessary excisions and scars: Patients no longer bear the physical burden of redundant biopsies, which is particularly important for cosmetically sensitive areas like the face and hands.
- Patient worries about invasive testing: Clear visual records reassure patients that their lesions are stable, easing anxiety and reducing insistence on unnecessary procedures.
- Costs from avoidable procedures: Practices save money on pathology fees and operating room time, while patients benefit from lower out-of-pocket costs.
Reducing biopsies doesn’t just benefit patients—it also streamlines the dermatologist’s workflow. By cutting down on unnecessary procedures, providers can focus on high-priority cases and urgent diagnoses. The practice also avoids overburdening pathology partners with benign samples, improving overall efficiency in the care chain.
Case example: A middle-aged patient is concerned that a mole on her inner thigh looks different. Using her mapped history, the dermatologist shows that the lesion has been stable for three years. The patient is reassured, no biopsy is performed, and unnecessary scarring is avoided.
Better Communication Across Providers and Pathology
Mapped lesions integrate directly with ICD-10, CPT, and SNOMED codes, ensuring:
- Surgeons excise the correct lesion with no guesswork: The precise anatomic location reduces the risk of wrong-site surgeries.
- Pathologists receive precise specimen correlation: Each biopsy specimen is matched to a coded lesion, minimizing confusion in pathology reports.
- All providers within the practice share standardized documentation—minimizing miscommunication and errors: Whether it’s a dermatologist, surgeon, or oncologist, everyone works from the same map.
A dermatology practice is rarely an island—patients often transition between multiple providers. Miscommunication about lesion identity can lead to dangerous mistakes, including missed diagnoses or incorrect treatments. By using accurate 3D body map documentation, dermatologists create a seamless bridge of communication that protects both the patient and the practice.
Case example: A dermatologist refers a patient for surgical excision of a lesion hidden behind the ear. The 3D body map highlights the exact spot with coded precision, ensuring the surgeon removes the correct lesion and the pathologist receives an accurate correlation.
Stronger Billing, Compliance, and Legal Protection
3D body map charting strengthens practice operations by:
- Supporting accurate claims submission and fewer denials: Properly coded lesion data ensures that every documented diagnosis and procedure aligns with payer requirements.
- Creating defensible records for audits or litigation: Detailed maps show a high standard of care and diligence in documentation, which is invaluable in audits or malpractice cases.
- Building a compliant, standardized charting structure: 3D mapping reduces variability in how clinicians document, helping practices maintain consistent records across the board.
Proper coding is the key to reliable reimbursement. Many denied claims result not from lack of medical necessity but from incomplete or vague documentation. 3D maps solve this by linking lesions directly to standardized codes, reducing ambiguity and improving the likelihood of payment. For practices, this means a more predictable revenue stream and fewer hours spent appealing denials.
Case example: During an insurance audit, a practice is asked to justify multiple lesion removals. The 3D maps clearly show each lesion’s exact location, its corresponding ICD-10 and CPT codes, and documented changes over time. This precise coding ensures the claims are paid promptly and withstand payer scrutiny.
How 3D Body Maps Engage Patients in Their Own Care
Patients understand visuals better than narrative notes. When shown their mapped lesions, patients can:
- Monitor changes at home: Patients can track their own lesions more confidently between visits.
- Better grasp the importance of follow-up: Seeing progression or stability visually reinforces why regular check-ups matter.
- Participate in shared decision-making: Patients are more engaged when they can clearly see the rationale for observation versus intervention.
Dermatologists often face challenges in convincing patients to return for follow-ups or to avoid unnecessary worry. 3D maps turn the abstract into concrete—patients can literally see what the dermatologist sees. This shared perspective not only improves compliance but also enhances satisfaction, making patients feel like active participants in their care.
Case example: A patient hesitant about scheduling regular follow-ups changes his mind after seeing a clear side-by-side comparison of his mapped lesions. The visualization makes him realize how important ongoing surveillance is for his health.
FAQ
How is 3D body maps different from 2D body maps?
2D body maps are a flat representation of a body. 3D body maps mimic the body, providing exact anatomic localization and coding, making data standardized and reproducible.
Does it take longer to document with a 3D body map?
No—point-and-click mapping often reduces charting time compared to writing lengthy narrative descriptions.
Can 3D body maps really reduce biopsies?
Yes. By clearly showing whether a lesion is stable or new, providers avoid biopsies driven by uncertainty.
How does 3D body maps affect billing?
Integrated coding ensures accurate claims submission, fewer denials, and stronger audit protection.
Will patients actually engage with 3D body maps?
Yes—seeing their own mapped lesions improves understanding and makes at-home monitoring easier.
Key Takeaways
- 3D body maps localize lesions with precise anatomic accuracy—even in hard-to-document areas like behind the ear, between the fingers, or inside the mouth.
- Longitudinal mapping enables earlier melanoma detection.
- Practices reduce unnecessary biopsies and patient anxiety.
- Properly coded lesion data strengthens billing accuracy, improving reimbursement and compliance.
- Patients engage more effectively with visual documentation.
Conclusion
3D body mapping isn’t just a documentation upgrade—it’s a clinical advantage. For dermatologists, it means stronger compliance, reduced liability, more efficient workflows, and a measurable impact on patient outcomes. Practices that adopt this technology aren’t just keeping better records—they’re elevating their standard of care.
Request a Demo
